Involuntary loss of urine or Urinary Incontinence
Urinary Incontinence in Women
Millions of women experience involuntary loss of urine called urinary incontinence (UI). Some women may lose a few drops of urine while running or coughing. Others may feel a strong, sudden urge to urinate just before losing a large amount of urine. Many women experience both symptoms. UI can be slightly bothersome or totally debilitating. For some women, the risk of public embarrassment keeps them from enjoying many activities with their family and friends. Urine loss can also occur during sexual activity and cause tremendous emotional distress.
Women experience UI twice as often as men. Pregnancy and childbirth, menopause, and the structure of the female urinary tract account for this difference. But both women and men can become incontinent from neurologic injury, birth defects, stroke, multiple sclerosis, and physical problems associated with aging.
Older women experience UI more often than younger women. But incontinence is not inevitable with age. UI is a medical problem. Incontinence occurs because of problems with muscles and nerves that help to hold or release urine. The body stores urine—water and wastes removed by the kidneys—in the bladder, a balloon-like organ. The bladder connects to the urethra, the tube through which urine leaves the body.
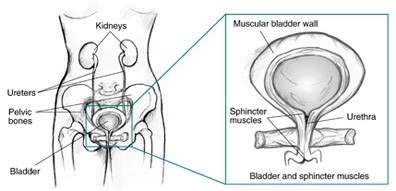
Figure: Front view of female urinary tract.
During urination, muscles in the wall of the bladder contract, forcing urine out of the bladder and into the urethra. At the same time, sphincter muscles surrounding the urethra relax, letting urine pass out of the body. Incontinence will occur if your bladder muscles suddenly contract or the sphincter muscles are not strong enough to hold back urine. Urine may escape with less pressure than usual if the muscles are damaged, causing a change in the position of the bladder. Obesity, which is associated with increased abdominal pressure, can worsen incontinence. Fortunately, weight loss can reduce its severity.
What are the types of incontinence?
Stress Incontinence
If coughing, laughing, sneezing, or other movements that put pressure on the bladder cause you to leak urine, you may have stress incontinence. Physical changes resulting from pregnancy, childbirth, and menopause often cause stress incontinence. This type of incontinence is common in women and, in many cases, can be treated.
Childbirth and other events can injure the scaffolding that helps support the bladder in women. Pelvic floor muscles, the vagina, and ligaments support your bladder. If these structures weaken, your bladder can move downward, pushing slightly out of the bottom of the pelvis toward the vagina. This prevents muscles that ordinarily force the urethra shut from squeezing as tightly as they should. As a result, urine can leak into the urethra during moments of physical stress. Stress incontinence also occurs if the squeezing muscles weaken.
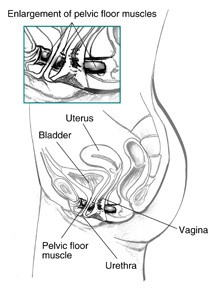
Figure: Side view of female pelvic muscles
Stress incontinence can worsen during the week before your menstrual period. At that time, lowered estrogen levels might lead to lower muscular pressure around the urethra, increasing chances of leakage. The incidence of stress incontinence increases following menopause.
Urge Incontinence
If you lose urine for no apparent reason after suddenly feeling the need or urge to urinate, you may have urge incontinence. A common cause of urge incontinence is inappropriate bladder contractions. Abnormal nerve signals might be the cause of these bladder spasms.
Urge incontinence can mean that your bladder empties during sleep, after drinking a small amount of water, or when you touch water or hear it running (as when washing dishes or hearing someone else taking a shower). Certain fluids and medications such as diuretics or emotional states such as anxiety can worsen this condition. Some medical conditions, such as hyperthyroidism and uncontrolled diabetes, can also lead to or worsen urge incontinence.
Involuntary actions of bladder muscles can occur because of damage to the nerves of the bladder, to the nervous system (spinal cord and brain), or to the muscles themselves. Multiple sclerosis, Parkinson's disease, Alzheimer's disease, stroke, and injury—including injury that occurs during surgery—all can harm bladder nerves or muscles.
Overactive Bladder
Overactive bladder occurs when abnormal nerves send signals to the bladder at the wrong time, causing its muscles to squeeze without warning. Voiding up to seven times a day is normal for many women, but women with overactive bladder may find that they must urinate even more frequently.
Specifically, the symptoms of overactive bladder include
- urinary frequency—bothersome urination eight or more times a day or two or more times at night
- urinary urgency—the sudden, strong need to urinate immediately
- urge incontinence—leakage or gushing of urine that follows a sudden, strong urge
- nocturia—awaking at night to urinate
Functional Incontinence
People with medical problems that interfere with thinking, moving, or communicating may have trouble reaching a toilet. A person with Alzheimer's disease, for example, may not think well enough to plan a timely trip to a restroom. A person in a wheelchair may have a hard time getting to a toilet in time. Functional incontinence is the result of these physical and medical conditions. Conditions such as arthritis often develop with age and account for some of the incontinence of elderly women.
Overflow Incontinence
Overflow incontinence happens when the bladder doesn't empty properly, causing it to spill over. Your doctor can check for this problem. Weak bladder muscles or a blocked urethra can cause this type of incontinence. Nerve damage from diabetes or other diseases can lead to weak bladder muscles; tumors and urinary stones can block the urethra. Overflow incontinence is rare in women.
Mixed Incontinence
Stress and urge incontinence often occur together in women. Combinations of incontinence—and this combination in particular—are sometimes referred to as mixed incontinence. Most women don't have pure stress or urge incontinence, and many studies show that mixed incontinence is the most common type of urine loss in women.
Transient incontinence
Transient incontinence is a temporary version of incontinence. Medications, urinary tract infections, mental impairment, and restricted mobility can all trigger transient incontinence. Severe constipation can cause transient incontinence when the impacted stool pushes against the urinary tract and obstructs outflow. A cold can trigger incontinence, which resolves once the coughing spells cease.
|
The Types of Urinary Incontinence
|
|
Stress
|
Leakage of small amounts of urine during physical movement (coughing, sneezing, exercising).
|
|
Urge
|
Leakage of large amounts of urine at unexpected times, including during sleep.
|
|
Overactive Bladder
|
Urinary frequency and urgency, with or without urge incontinence.
|
|
Functional
|
Untimely urination because of physical disability, external obstacles, or problems in thinking or communicating that prevents a person from reaching a toilet.
|
|
Overflow
|
Unexpected leakage of small amounts of urine because of a full bladder.
|
|
Mixed
|
Usually the occurrence of stress and urge incontinence together.
|
|
Transient
|
Leakage that occurs temporarily because of a situation that will pass (infection, taking a new medication, colds with coughing).
|
How is incontinence evaluated?
An Urogynecologist is a doctor who focuses on urinary and associated pelvic problems in women. And who has experience in treating incontinence
Your Urogynecologist will physically examine you for signs of medical conditions causing incontinence, including treatable blockages from bowel or pelvic growths. In addition, weakness of the pelvic floor leading to incontinence may cause a condition called prolapse, where the vagina or bladder begins to protrude out of your body. This condition is also important to diagnose at the time of an evaluation.
Your Urogynecologist may also recommend other tests:
- Urinalysis and urine culture—Laboratory technicians test your urine for evidence of infection, urinary stones, or other contributing causes.
- Ultrasound— This test uses sound waves to create an image of the kidneys, ureters, bladder, and urethra.
- Cystoscopy— The doctor inserts a thin tube with a tiny camera in the urethra to see inside the urethra and bladder.
- Urodynamics— Various techniques measure pressure in the bladder and the flow of urine.
How is incontinence treated?
Fortunately, there are many treatments for urinary incontinence.
Recommended Related to Urinary Incontinence/OAB
The Truth About Urine
Urine isn't something most people talk about. We barely give it more than a passing glance as it swirls out of sight down the toilet bowl. Yet changes in the urine -- its color, odor, and consistency -- can provide important clues about the status of your body. Your urine can reveal what you've been eating, how much you've been drinking, and what diseases you have. "Urine and urinalysis have, for hundreds of years, been one of the ways physicians have looked at health," says Tomas Griebling, MD,...
- Behavioral treatment. Some people with urinary incontinence may get relief by making simple lifestyle changes. If you have stress incontinence, for instance, in which you leak urine when you cough, sneeze, or laugh, your doctor may tell you to limit how much you drink. If you have urge incontinence, in which you get the sudden urge to urinate and can't always make it to the bathroom in time, your doctor may tell you to avoid spicy foods, caffeine, and carbonated drinks, because they can irritate the bladder and make the problem worse. Exercises to strengthen the pelvic floor muscles, known as Kegels, can sometimes help people with stress incontinence. Kegels can also help people with urge incontinence. For urge incontinence, bladder training, can also help. This involves gradually increasing the interval time between trips to the bathroom, working up to longer and longer intervals between bathroom stops.
- Drugs. For urge incontinence, medications known as anticholinergics/ antimuscarinics can prevent bladder spasms.
- Devices and absorbent products. Protective pads and panty liners can help avoid embarrassing situations. A pessary, a plastic device inserted into the vagina, may help prevent urine leakage by supporting the neck of the bladder; it is most useful for stress incontinence.
- Surgery. If the above treatments don't provide enough relief, surgery may help.
Surgery for Stress Incontinence
In some women, the bladder can move out of its normal position, especially following childbirth. Surgeons have developed different techniques for supporting the bladder back to its normal position. The three main types of surgery are retropubic suspension and two types of sling procedures.
Retropubic suspension uses surgical threads called sutures to support the bladder neck. The most common retropubic suspension procedure is called the Burch procedure. In this operation, the surgeon makes an incision in the abdomen a few inches below the navel and then secures the threads to strong ligaments within the pelvis to support the urethral sphincter. This common procedure is often done at the time of an abdominal procedure such as a hysterectomy.
Sling procedures are performed through a vaginal incision. The traditional sling procedure uses a strip of your own tissue called fascia to cradle the bladder neck. The surgeon attaches both ends of the sling to the pubic bone or ties them in front of the abdomen just above the pubic bone. Midurethral slings are newer procedures that use synthetic mesh materials that the Urogynaecologist surgeon places midway along the urethra. The two general types of midurethral slings are retropubic slings, such as the transvaginal tapes (TVT), and transobturator slings (TOT).
If you have pelvic prolapse, your surgeon may recommend an anti-incontinence procedure with a prolapse repair and possibly a hysterectomy.
Finally, many women are afraid to mention their problem. They may have urinary incontinence that can improve with treatment but remain silent sufferers and resort to wearing absorbent undergarments, or diapers. This practice is unfortunate, because diapering can lead to diminished self-esteem, as well as skin irritation and sores. If you are relying on diapers to manage your incontinence, you and your family should discuss with your doctor the possible effectiveness of treatments such as timed voiding and pelvic muscle exercises.